Demystifying Pudendal Nerve Issues
Pudendal neuralgia (PN) is a nerve pain condition caused by damage, injury, inflammation, or irritation somewhere along the pudendal nerve pathway. PN can be a debilitating condition which impacts quality of life, bladder and bowel function, sexual function, mental health, and physical health.
Patients with PN frequently complain of chronic perineal and/or genital pain which can be exacerbated by sitting or hip flexion movements (i.e squats, bending over, etc). It would likely feel like a burning, tingling, aching, stabbing, or electric shock-like type pain. Patients with PN may also complain of tailbone pain, sciatic nerved pain, pain with bowel movements & constipation, pain with sexual activity, ejaculation, & ED issues, and/ or decreased genital sensation especially during sexual activity. Sometimes patients also notice overactive bladder symptoms (urinary urgency and frequency) and constipation as well. Oftentimes, pain is relieved by laying down, standing, or sitting on the toilet - all positions that reduce pressure along the pudendal nerve pathway.
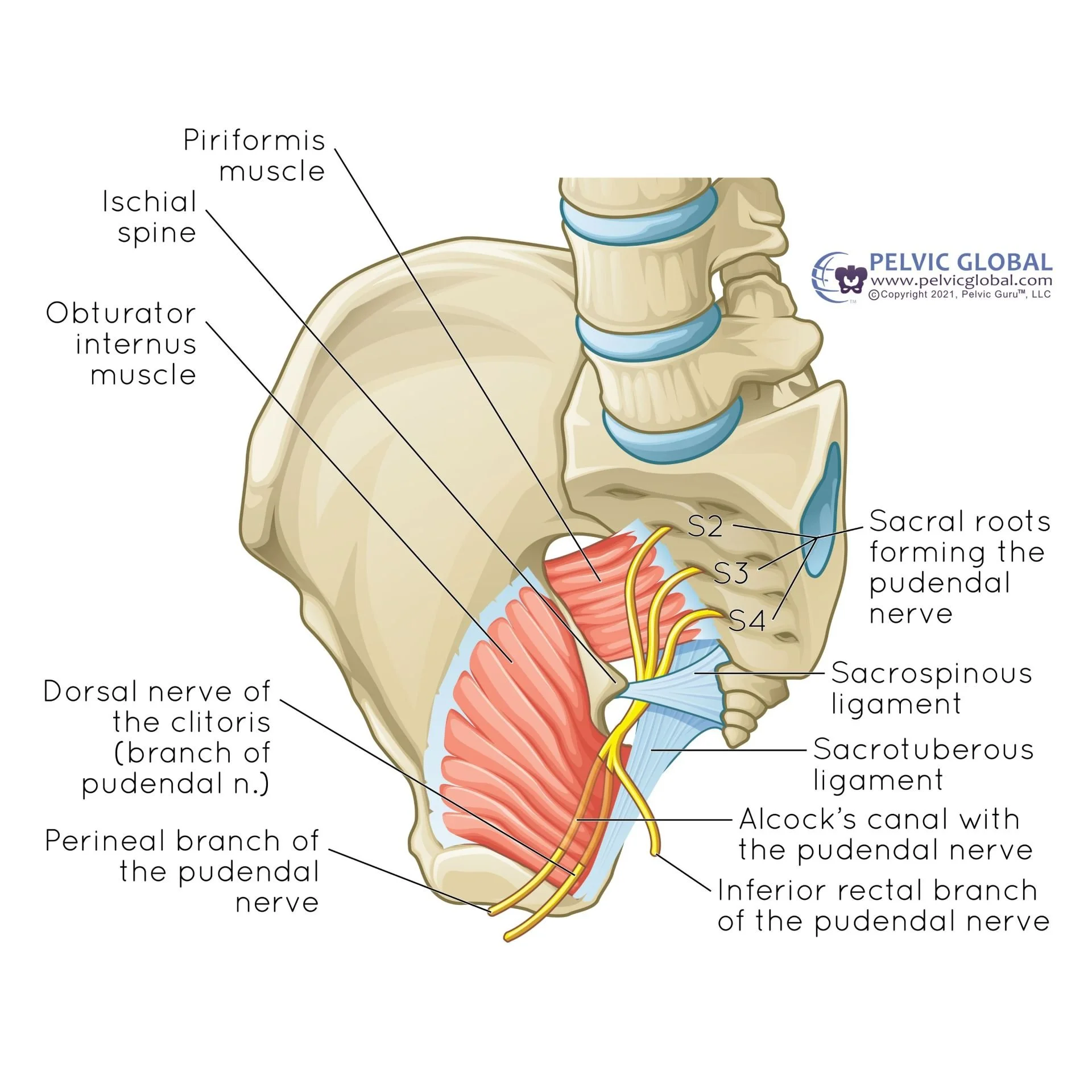
Pudendal Nerve Pathway
PN is typically caused by cumulative, repetitive microtrauma to the nerve. But it may also be caused by acute trauma or injuries due to childbirth, falls, car accidents, and pelvic surgeries (eg, pelvic organ prolapse repairs with mesh). Risk factors that may contribute to developing PN are chronic constipation, prolonged sitting pelvic radiation therapy due to cancer treatments, and repetitive hip flexion activities (cycling, squats). It’s also important to mention that stress can impact PN. Although stress does not directly involve the nerve, it is a powerful aggravator of neuropathic pain.
PN & Pudendal Nerve Entrapment (PNE) are related but distinctly different. PN is nerve irritation & pain which is caused by a transient issue and symptoms may come & go. The main causes of PNE would be congenital - if the nerve passes through muscle or fascia that it shouldn’t, or traumatic - due to an injury to the nerve such as a fall or car accident, or due to a pelvic surgery (usually pelvic organ prolapse repair). If the cause is traumatic, it could be because of direct injury to the nerve (usually felt immediately after the initial injury or surgery) or from development of scar tissue along the nerve pathway which could take months to develop. Only 1% of PN cases are true entrapment - most often is pudendal neuralgia without entrapment. Pelvic Physical Therapy can help manage symptoms of PNE, but ultimately surgical decompression. Other medical treatments for PN or PNE would be pain medications (NSAIDs, gabapentin, amitriptyline) muscle relaxers (cyclobenzaprine), botox injections to surrounding pelvic floor muscles, pudendal nerve blocks, and finally a surgically implanted pain management device (interstim or DRG stimulator).
It’s important to try conservative care treatments before progressing to invasive medical care. Pelvic Physical Therapy can be curative for managing symptoms of PN. Treatments include pelvic floor muscle lengthening, tissue & nerve desensitization techniques, lifestyle modifications (sitting on a donut cushion and reducing overall time spent sitting), improving hip mobility, myofascial release and mobilization, & sacral neuromodulation (I like to do this by Dry Needling near the sacral nerves (S2-4) combined with electric stimulation therapy). Pain management techniques are crucial for these patients, especially in the beginning phases of recovery. Doing diaphragmatic/ 360 breathing, mindfulness and meditation, and using an at home TENS unit are all effective strategies. Once the pain is more manageable, transitioning to pelvic girdle strengthening is important. Focusing on the muscles that support and stabilize the pelvis can help take unnecessary strain off the pelvic nerves and pelvic floor muscles.
For exercises start with gentle stretching & mobility that includes:
Puppy dog pose
Cat/cow
Figure 4 Rockers
Happy baby or single leg happy baby
Hip Internal Rotation
Frog pose to child’s pose
You can find a video of all the exercises here: https://www.instagram.com/reel/DXb6T4vB71w/?utm_source=ig_web_copy_link&igsh=MzRlODBiNWFlZA==
CITATIONS:
Leslie SW, Antolak S, Feloney MP, et al. Pudendal Neuralgia. [Updated 2024 Feb 12]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK562246/
Heather Edwards, Dr. Tracy Sher. Pudendal Neuralgia and Entrapment: Clinical Pearls. Pelvic Global: Expert Webinar Series.
Images used with permission from Pelvic Guru®, LLC as a Pelvic Global Member