Understanding Chronic Pain
Pelvic pain can significantly affect your quality of life, relationships, physical health, mental health, and more. Pelvic pain issues are very often underdiagnosed or misdiagnosed as something else. You may have been told you had a UTI or Prostatitis and taken antibiotics over an over again with no resolution in your symptoms. You may have had pain with intercourse for years and have been told to “just have a drink and relax.” You may have other diagnoses that increase your risk of pelvic pain, like Interstitial Cystitis, Endometriosis, true bacterial UTI or Prostatitis, IBS, etc. If that sounds familiar, this blog post was written specifically for you.
In order to get out of pain, it is crucial to understand how pain actually works. Pain is a normal experience, but living in pain is not normal. The medically accepted definition of pain is “an unpleasant sensory and emotional experience associated with, or resembling that associated with, actual or potential tissue damage.” The interesting thing about this definition is that it implies that actual tissue damage is not required for something to be considered painful. Just the “potential” for tissue damage may be enough for your brain to trigger a pain response. It is important to recognize that most stimuli which cause pain might actually damage tissue, which would cause an unpleasant physical sensation in the body. Pain is also always unpleasant and therefore considered to be an emotional experience as well.
There are two types of pain: acute pain and persistent (or chronic) pain.
Acute pain usually begins suddenly because of an injury. The pain goes away once you’ve healed. Healing usually doesn’t take longer than 3 to 6 months. Acute pain is necessary for survival - it alerts us that something is wrong that needs our attention.
Persistent pain lasts beyond the time needed for healing. In these cases, the pain is no longer useful.
With persistent pain, your body has fully healed from an initial injury, but the nerves (your body’s alarm system) have become extra sensitive. When this happens, it only takes a little bit of movement, activity, or change in emotion to set off your sensitive alarm system and causes pain. Your body isn’t in danger. It’s just that your nerves have changed the way they respond to normal sensations - making you hypersensitive to pain. It’s like a fire alarm going off when there is no fire - and every time you treat the alarm like an emergency, you reinforce the belief that your body is fragile. So you move less, avoid doing things you need to or would like to do, & stay stuck in the flare-up cycle.
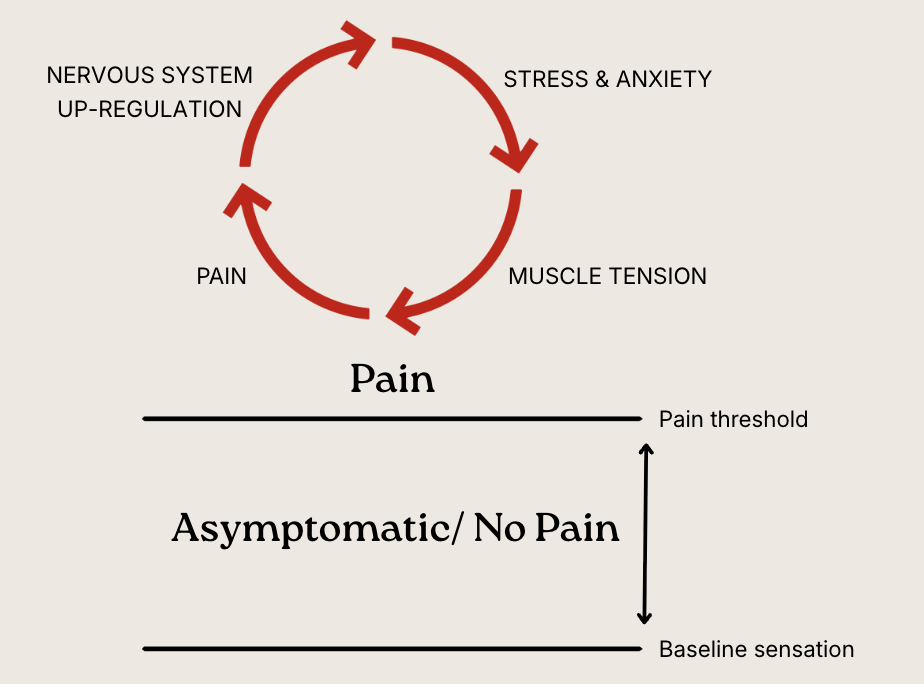
Pain works on a threshold. Everywhere above the threshold is “pain,” or symptoms. Everywhere below the threshold, is no pain or “asymptomatic.” Usually people live somewhere between baseline sensation & the pain threshold at any given time. When someone has persistent, chronic, pain they live very near to, or above the pain threshold at all times. When you live in constant pain, it increases nervous system activity, leading to increased anxiety & stress, further increasing muscle tension, which causes more pain - it’s a vicious cycle. The goal is to break the cycle in multiple points along the chain so that it’s less likely to repeat itself. This can refocus your attention away from the pain and ultimately train your brain to “dial down” the pain. We want to get you far enough below the pain threshold, so that something as “small” as sitting or physical activity doesn tcause a flare-up.
There are 3 categories of treatments to focus on to break the cycle: Physical, Mental, and Medical. There can be crossover between items in each category. Ideally we want to treat pain without, or with the least amount, of medication, but it is there for a reason and should be used cautiously if needed.
Physical
Slowly & gently increasing movement around the painful area in order to allow your brain & body to become comfortable with physical activity.
This may include stretching, strengthening, dry needling, electric stimulation, massage, myofascial mobilization, cupping, heat/ice, red light therapy, etc.
Mental
Stress management, meditation, sleep, breathing exercises, etc.
Medical
Pain medication, muscle relaxers, injections, nerve blocks, surgical procedures,etc.
Stay tuned for more information on chronic pain & pelvic pain. Please email restorepelvicrehab@gmail with any questions.
x, Dr. Bethany