Urinary Incontinence After Prostate Cancer Treatment
Urinary leakage after prostate cancer treatment is common — but it’s rarely talked about. If you or someone you know, has been through prostate cancer treatment and is now dealing with urinary leakage — you are not alone and this is very common. This is especially true if there was surgical intervention (RALP - Robotic-Assisted Laparoscopic Prostatectomy), but this can still be the case with other cancer treatments like radiation.
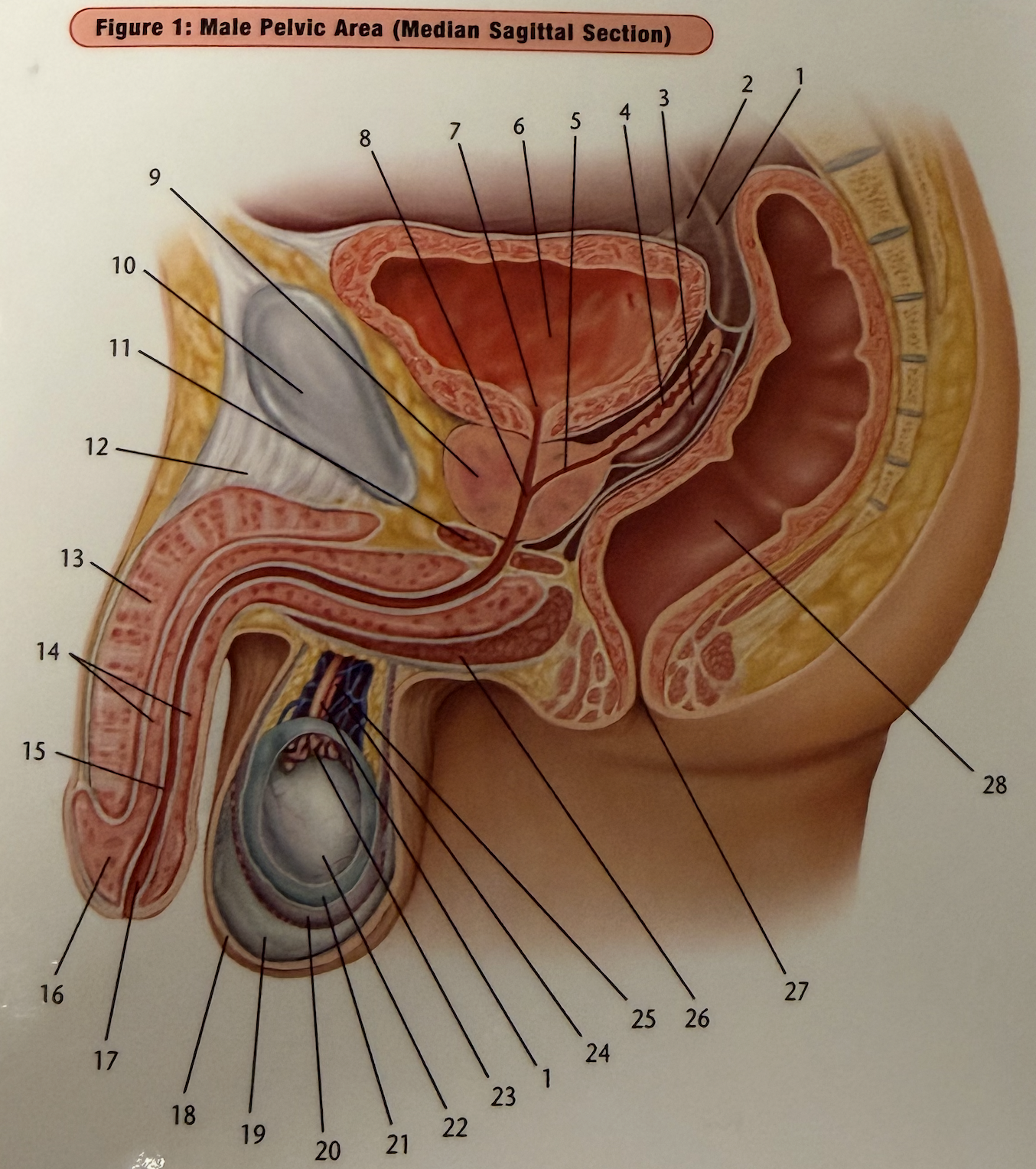
The prostate is located just below the bladder and right above the pelvic floor muscles. The main function of the prostate is to produce seminal fluid. Muscles within the prostate also assist in controlling urine flow and ejaculation. (1) The muscles within the prostate are not under voluntary control, but the muscles of the pelvic floor, including the urinary sphincter, are under voluntary control.
The most common type of urinary leakage after prostate cancer treatment is “stress urinary incontinence” (SUI). SUI happens when an increase in pressure in the stomach squishes the bladder, and if the urinary sphincter and pelvic floor muscles are not quick enough or strong enough to contract against the pressure, it can cause leakage. The main cause of urinary leakage after prostate cancer treatment is a problem with urinary sphincter control - weakness, poor coordination, or poor endurance. Some pre-existing conditions that may affect speed and completeness of recovery are increased age, diabetes, obesity and higher BMI, lower rates of physical activity, pre-existing overactive bladder issues, and having an enlarged prostate. (2)
With normal male pelvic anatomy, the prostate surrounds part of the urethra and contributes to urinary continence by providing structural support. During prostatectomy surgery, the surgeon removes the prostate along with the urethra inside. Then they suture the two ends of the urethra together. This is where the internal stitches are located and why people have a catheter after surgery. After surgery, the urethra is shortened and the internal sphincter mechanism is altered, which means the external sphincter and pelvic floor must work much harder to maintain control.
After prostatectomy, several factors contribute to urinary leakage. The urethra is shortened, the internal sphincter is altered, and the external sphincter becomes the primary structure responsible for continence. First, because the prostate is no longer there putting constant pressure on the urethra, the pelvic floor and urinary sphincter have to compensate and squeeze harder due to the lack of “help.” If the muscles are not strong enough, coordinated enough, or don’t have good endurance, it will limit how effectively they can compensate for the lack of the prostate. Due to the trauma of the surgery the muscles often do not function properly. Another reason leakage occurs after surgery is that the bladder may continue to contract with the same force it used before. Without the prostate’s structural support and with a recovering sphincter, those bladder contractions can overwhelm the pelvic floor muscles — contributing to urgency, frequency, and urge-related leakage.
Radiation treatment affects the pelvis in a slightly different way. The prostate is not removed, rather radiation damages the cancer cells enough so that they don’t reproduce or replicate. Because the urinary sphincter sits very close to the prostate, this muscle can be affected during radiation treatment. Radiation can affect muscle tissue, surrounding nerves, and blood supply — which may reduce sphincter strength, coordination, and endurance over time - leading to SUI.
Urinary leakage does not affect the urinary system alone. Research shows urinary leakage significantly impacts quality of life — affecting physical activity, confidence, social interactions, work, and emotional wellbeing. Most individuals undergoing prostatectomy will experience some degree of urinary leakage immediately after surgery. The severity and duration of leakage varies from person to person. The average time to gaining full urinary control back after surgery is about 3-6 months. (2) Pelvic health physical therapy can significantly improve speed of recovery, coordination, and confidence - you don’t have to just “wait it out.” Pelvic floor physical therapy also doesn’t have to just be after prostate cancer treatments, training before surgery (‘prehabilitation’) has been shown to improve early recovery of continence. You do not have to accept urinary leakage as the ‘new normal.’ With the right prehab & rehab, the pelvic floor can be retrained. If you or someone you love is planning prostate cancer treatment — or struggling after — schedule an evaluation with a pelvic health physical therapist trained in post-prostatectomy recovery. This is treatable.”
Citations:
InformedHealth.org [Internet]. Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); 2006-. In brief: How does the prostate work? [Updated 2022 Sep 15]. Available from: https://www.ncbi.nlm.nih.gov/books/NBK279291/
Gacci M, De Nunzio C, Sakalis V, Rieken M, Cornu JN, Gravas S. Latest Evidence on Post-Prostatectomy Urinary Incontinence. J Clin Med. 2023 Feb 2;12(3):1190. doi: 10.3390/jcm12031190. PMID: 36769855; PMCID: PMC9917389.